Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Discover what knee surgery really feels like, the pain timeline, crucial prep and recovery tips—but what do most patients wish they knew?
Worried about knee surgery? You’ll handle it better with a plan. Expect pressure and throbbing as the nerve block fades, worst the first night. Set up prehab, a med list, a couch “recovery station,” ice packs, and a walker. After, elevate, ice 20 minutes on/off, take meds on schedule, and walk short laps. Watch for fever or calf pain. Want the exact timeline—and what most people wish they knew?
In plain terms: yes, you’ll feel pain after knee surgery—but it’s manageable, predictable, and it changes fast over the first week. Right after surgery, you’ll feel pressure, throbbing, and a tight, hot ache. The numbing medicine and nerve block help for 12–24 hours, then pain peaks the first night and next morning. Don’t panic—plan. Take scheduled meds before the block wears off, use ice 15–20 minutes at a time, elevate above your heart, and keep the bandage dry and snug, not strangling.
Expect swelling, bruises, and stiffness that make bending sting. Short walks every couple of hours, heel slides, and calf pumps reduce stiffness and clots. Pace yourself: pain 3–5 out of 10 is fine during exercises; sharp, tearing pain is a stop sign. Sleep can be cranky, so stack pillows under your calf, not the knee. Protein, fluids, and fiber fight fatigue and constipation. Rest helps too.
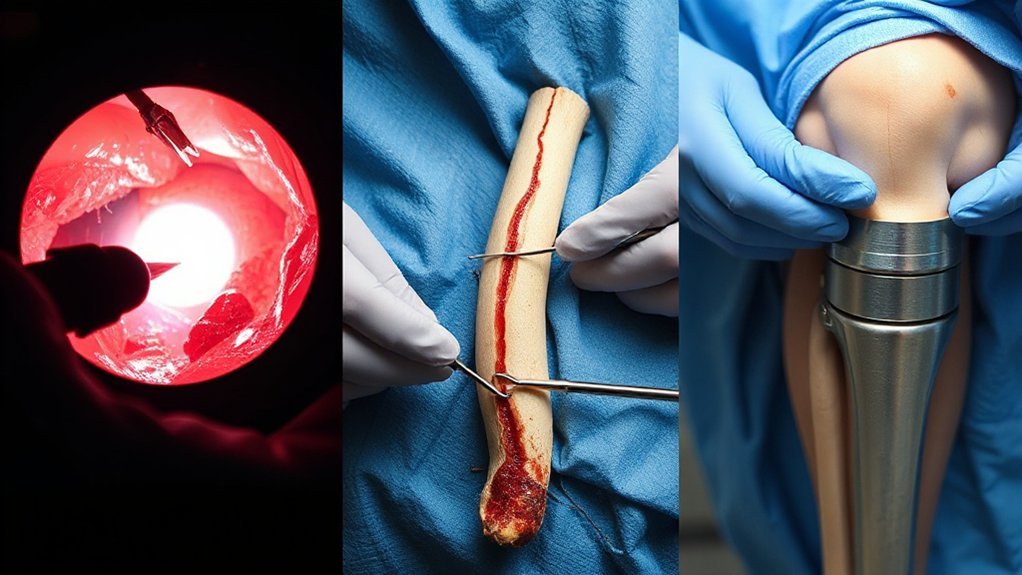
You’ll want to know what each surgery tries to fix and how big it is: arthroscopy uses small incisions to trim or repair cartilage or a meniscus, ACL reconstruction replaces a torn ligament with a graft, and total knee replacement resurfaces bone and swaps in metal and plastic. Recovery shifts a lot—arthroscopy can get you back to desk work in a few days and sports in 4–8 weeks, ACL rehab runs about 6–9 months, and a knee replacement often takes 3–6 months for daily life and up to a year for full strength. Risks rise with scope: arthroscopy has lower rates but still infection, clots, stiffness; ACL adds graft failure and motion loss; replacement adds clots, infection, implant loosening, and possible revision—so you match goals, timeline, and risk with your surgeon, no guesswork.
Before we talk recovery, let’s get clear on what each knee surgery aims to do—and how far it goes.
Arthroscopy is the tune‑up. Through portals, your surgeon inserts a camera, trims a torn meniscus, smooths frayed cartilage, removes loose bodies, or repairs tears. Goal: relieve catching and restore motion while keeping your original parts.
ACL reconstruction is the stability fix. The torn ligament isn’t stitched; it’s replaced with a graft—hamstring, patellar tendon, quad, or donor—through bone tunnels to recreate the ACL’s path. Result: pivoting, fewer “give‑way” moments.
Total knee replacement is the overhaul. Surgeons resurface the joint, removing damaged cartilage and bone, correcting alignment, and balancing ligaments. Metal and polyethylene components create bearing surfaces, sometimes with a patellar button. Aim: function when arthritis dominates.
Though the fixes differ, recovery follows a predictable arc: small scope, medium rebuild, big overhaul. After arthroscopy, you’re walking the day of surgery, driving in a few days, and jogging by weeks 4–6. ACL reconstruction asks more: crutches 1–2 weeks, running at 3 months, pivot sports around 9–12. Total knee replacement resets the clock: walker days, cane weeks, solid strides by 3 months, full confidence at 6–12.
Ask questions, adjust, keep showing up.

Getting ready starts now: prehab to build strength, meds to plan, and a home that makes moving easy. Build quads, glutes, and core with straight‑leg raises, mini squats to a chair, bridges, and ankle pumps, 3–4 days a week. Practice knee extension: towel under heel, relax, let gravity help. Stretch calves and hamstrings, steady. If you use a cane or walker, rehearse with it now. Your future self will thank you.
Med prep: list every prescription, supplement, and allergy. Ask which drugs to stop—blood thinners, anti‑inflammatories, some herbs—and when. Refill pain meds, stool softener, and anti‑nausea options, so you’re not scrambling. Set alarms for doses, and label pill boxes by day. Home setup: clear pathways, tape down cords, add nightlights. Put a sturdy chair with arms, a raised toilet seat, and a shower chair in place. Stock easy meals, ice packs, and zip bags. Pet gate? Yes, please.
You’ve prepped your body and your home; now it’s go-time. You arrive early, check in, swap clothes for a gown, and meet two key players: anesthesia and nursing. They confirm your history, allergies, and last meal, place an IV, clip the knee if needed, and mark the surgical site with ink. You sign consent, get an ID band, and breathe. Nerves are normal.
Early arrival, gown on, meet your team. ID, ink, breathe—nerves normal.
In the first 24 hours, expect manageable pain, a heavy, tight knee, and a clear plan. Nurses set your meds on schedule, you ice every hour, and you wiggle toes like it’s your job. You’ll stand with help, shuffle a few steps with a walker. Eat, hydrate, breathe.
Days 2–7, keep pain steady: take meds on time, don’t “tough it out.” Elevate above heart, 20 minutes on, 20 off with ice, cycles daily. Bandage stays clean and dry. You start gentle quad sets, ankle pumps, heel slides. Range of motion goal by the end of week one: 0–70° bend, near-straight extension. Stairs? One step at a time, rail and cane.
Weeks 2–4, swelling gradually fades, bruising spreads, clears. You switch to acetaminophen or NSAIDs if allowed, taper opioids. PT ramps up: stationary bike rocking to full turns, sit-to-stands, short walks outside. Milestones: full extension, 90°–110° flexion, steady gait.
As the swelling eases and the bike starts to turn, the job shifts: protect your gains and avoid the potholes. Risks? Infection, blood clots, scar stiffness, flare‑ups from doing too much, too soon. Red flags you don’t ignore: fever over 101°F, calf pain or sudden swelling, chest tightness, wound drainage that’s cloudy or foul, redness spreading, pain that’s worsening, numb foot.
Here’s how you stack the odds in favor:
1) Move smart: heel slides, quad sets, and walks, 5–10 minutes, 3–5 times daily. Elevate above heart, ice 15–20 minutes, every 2–3 hours. Add bike spins, low resistance, no hero turns.
2) Guard the wound: clean, dry dressing; shower, don’t soak; no lotions until cleared. Watch the edges daily, snap a photo log.
3) Protect the system: take anticoagulants as prescribed, wear compression, hydrate, protein at each meal, hit your sleep window, and keep pain controlled enough to move.
You’ve got this. Knee surgery isn’t a joyride, but it’s doable with a plan. Prep now: prehab exercises, meds list, freezer meals. Day one, expect throbbing as the block fades; set alarms, take meds on schedule. Ice 20 minutes, elevate above your heart, walk laps each hour. Protect the incision, keep it dry. Red flags? Fever over 101.5, calf pain, spreading redness—call. Then attend rehab, hit milestones, celebrate range. Step by step—back to real life.